Within the mid-Twentieth century, the invention of penicillin was hailed as a “miracle treatment.” It reworked once-fatal infections into manageable illnesses, extending the human lifespan by a long time. Nevertheless, the miracle is fading. We’re at present going through a worldwide well being disaster generally known as Antimicrobial Resistance (AMR).
Bacterial resistance to medication is a situation through which micro organism that have been beforehand inclined to antibiotics develop the power to outlive and multiply regardless of the presence of those self same medication. These “superbugs” render commonplace remedies ineffective, resulting in extended diseases, larger medical prices, and an elevated threat of dying.
Antibiotic Resistance: Hospital vs. Group
Whereas antibiotic resistance can happen anyplace, it’s considerably extra prevalent in hospital-acquired infections (nosocomial infections) than in community-acquired ones.
Why Hospitals are Hotbeds for Resistance
Selective Stress: Hospitals use huge portions of antibiotics. This atmosphere kills off inclined micro organism however permits resistant strains to outlive and thrive—a course of generally known as “choice.”
Weak Populations: Sufferers in hospitals typically have weakened immune methods or invasive gadgets (like catheters or ventilators), offering straightforward entry factors for resistant micro organism.
Transmission Hubs: Regardless of strict hygiene protocols, the excessive density of contaminated people and frequent contact with healthcare staff facilitate the unfold of hardy bacterial strains.
These hospital strains are significantly harmful as a result of they typically exhibit multidrug resistance (MDR), that means they’re proof against a number of completely different courses of antibiotics concurrently.
Widespread “Superbug” Strains
A number of particular micro organism have develop into infamous for his or her drug-resistant capabilities:
Staphylococcus aureus (MRSA): Typically immune to methicillin and different widespread penicillins.
Escherichia coli (E. coli): A Gram-negative enteric bacterium more and more immune to carbapenems, our “last-resort” antibiotics.
Pseudomonas aeruginosa: A resilient pathogen recognized for inflicting extreme lung and blood infections, typically exhibiting resistance to virtually all accessible remedies.
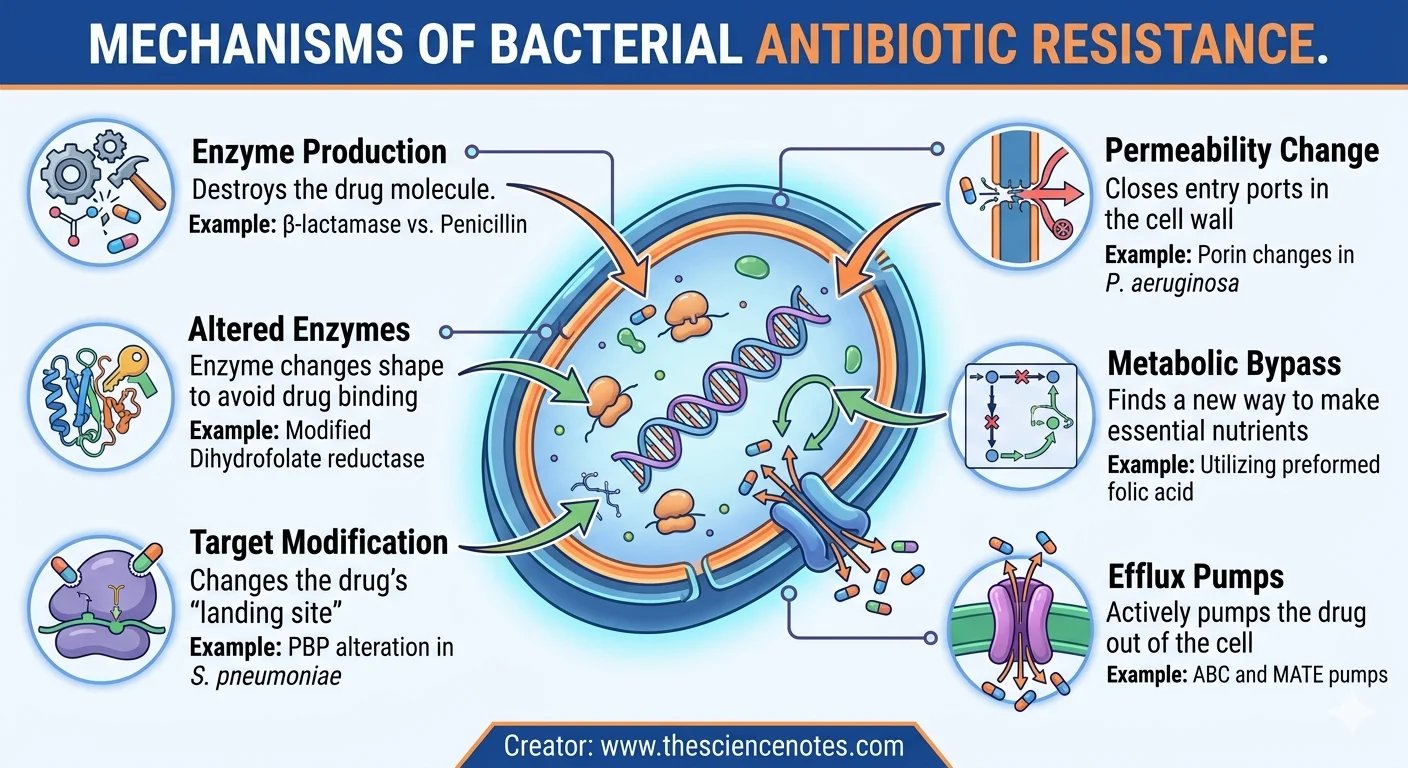
6 Key Mechanisms of Antibiotic Resistance
Micro organism are organic masters of adaptation. They make use of a number of subtle methods to neutralize the specter of antibiotics. Understanding these mechanisms is step one in growing new countermeasures.
1. Manufacturing of Inactivating Enzymes
The most typical manner micro organism combat again is by producing enzymes that bodily dismantle the antibiotic molecule earlier than it might do hurt.
Carbapenems: Historical past, Construction, Mechanism of Motion, resistance and Antimicrobial Exercise
Modifying Enzymes: Gram-negative micro organism typically carry plasmids that encode adenylating, phosphorylating, or acetylating enzymes. These chemically “tag” aminoglycoside antibiotics, stopping them from binding to their targets.
Aminoglycosides: Historical past, Construction, Antimicrobial Exercise, Mechanism of Motion, and Resistance
2. Manufacturing of Altered Enzymes
Typically, micro organism don’t destroy the drug; as a substitute, they alter the “lock” so the “key” (the drug) now not suits.
Instance: In trimethoprim-resistant micro organism, the enzyme dihydrofolate reductase is barely modified. The modified model can nonetheless carry out its important metabolic features however is now not inhibited by the drug.
3. Synthesis of Modified Targets
Antibiotics work by binding to particular buildings throughout the micro organism, reminiscent of ribosomes or cell wall proteins. Micro organism can change these targets to evade detection.
Ribosomal Modification: A methylated 23S ribosomal RNA could cause resistance to erythromycin. Equally, a mutation within the 50S ribosomal subunit can render streptomycin ineffective.
PBP Alteration: In S. pneumoniae, resistance to penicillin is commonly attributable to the loss or alteration of Penicillin-Binding Proteins (PBPs), that means the drug has nothing to latch onto.
4. Alteration of Cell Wall Permeability
If the drug can’t get into the cell, it might’t kill the micro organism. Many micro organism develop resistance by limiting entry.
Porin Modifications: P. aeruginosa can alter its porins (channel proteins), successfully closing the “doorways” to tetracyclines.
Pure Obstacles: Some micro organism, like Streptococci, have a pure permeability barrier that makes them inherently immune to aminoglycosides.
5. Alteration of Metabolic Pathways
If an antibiotic blocks a particular chemical response the micro organism have to survive, some micro organism merely discover a “detour.”
Instance: Sulfonamides work by stopping micro organism from making folic acid from PABA. Nevertheless, some resistant micro organism have advanced to bypass this requirement completely by using preformed folic acid from their atmosphere, very like human cells do.
6. Efflux Pumps: The Mobile “Ejector Seat”
Efflux pumps are specialised proteins positioned within the bacterial cell membrane that actively pump antibiotics out of the cell earlier than they will attain poisonous ranges.
Main Households: These embody the ABC (ATP-binding cassette) pumps, MATE (multidrug resistance and poisonous compound extrusion) pumps, and the MFSE (main facilitator superfamily efflux) pumps.
These pumps are sometimes answerable for resistance to a number of courses of medication, together with quinolones and aminoglycosides.
How Resistance Spreads: Bacterial Genetics
Micro organism don’t simply inherit resistance from their “mother and father”; they will additionally share resistance genes with their “neighbors” like a digital file switch.
Vertical Gene Switch (VGT)
That is generational inheritance. When a resistant bacterium divides, it passes its resistant genes all the way down to its daughter cells. By way of speedy replica, a single resistant cell can create a colony of tens of millions in a matter of hours.
Horizontal Gene Switch (HGT)
That is probably the most alarming side of antibiotic resistance, because it permits resistance to leap between completely different species of micro organism.
Transformation: Micro organism decide up fragments of DNA containing resistance genes from their surrounding atmosphere (typically left behind by lifeless micro organism).
Transduction: Resistance genes are carried from one bacterium to a different by a virus generally known as a bacteriophage.
Conjugation (Plasmid Switch): Typically known as “bacterial intercourse,” this includes the direct switch of round DNA molecules known as plasmids between micro organism. These plasmids typically carry “resistance cassettes” that include genes for resistance to a number of completely different antibiotics without delay.
The International Influence and the Want for Motion
The statistics are sobering. Tons of of hundreds of individuals die yearly globally from infections that have been as soon as simply treatable.
Observe: If left unchecked, it’s estimated that antimicrobial resistance might trigger 10 million deaths yearly by 2050, surpassing most cancers as a number one reason behind dying.
The Root of the Downside
The speedy improve in resistance is primarily pushed by:
Overuse: Prescribing antibiotics for viral infections (just like the widespread chilly or flu) the place they’ve zero impact.
Misuse: Sufferers failing to finish their full course of antibiotics, which permits the strongest micro organism to outlive and develop resistance.
Agricultural Use: The widespread use of antibiotics in livestock to advertise progress slightly than deal with illness.
The Path Ahead
To fight this “silent pandemic,” the worldwide group should intensify efforts in two key areas:
New Drug Improvement: We should incentivize the invention of latest courses of antibiotics and different therapies, reminiscent of phage remedy or monoclonal antibodies.
Stewardship: Implementing strict “antibiotic stewardship” packages in hospitals to make sure the best drug is used on the proper dose for the best length.
Abstract Desk: Mechanisms of Resistance
MechanismDescriptionExampleEnzyme ManufacturingDestroys the drug moleculebeta-lactamase vs. PenicillinAltered EnzymesEnzyme modifications form to keep away from drug bindingModified Dihydrofolate reductaseGoal ModificationModifications the drug’s “touchdown web site”PBP alteration in S. pneumoniaePermeability ChangeCloses entry ports within the cell wallPorin modifications in P. aeruginosaMetabolic BypassFinds a brand new solution to make important vitaminsUsing preformed folic acidEfflux PumpsActively pumps the drug out of the cellABC and MATE pumps
Conclusion
Bacterial resistance is a pure evolutionary course of, however human exercise has accelerated it to a harmful tempo. By understanding the advanced mechanisms—from enzyme manufacturing to efflux pumps—and recognizing how genetic materials is swapped by transformation and transduction, we are able to higher recognize the magnitude of this problem. The way forward for trendy drugs will depend on our skill to outsmart these microscopic adversaries by innovation, schooling, and accountable drug use.